Bioidentical Hormone Replacement Therapy vs Traditional Hormone Therapy – A Comparative Analysis

As women reach their 40s and beyond, hormone levels naturally decline, often leading to distressing symptoms such as hot flashes, mood swings, and disrupted sleep. For those grappling with these changes, hormone replacement therapy offers a way to alleviate symptoms and restore hormonal balance. Bioidentical hormone replacement therapy (BHRT) has gained attention as a potentially more natural alternative to traditional hormone therapies.
Understanding the nuances between BHRT and traditional hormone therapy is critical for women making informed decisions about their health. In this article, we will explore the intricacies of each approach, their efficacy, safety, and how individual factors influence treatment choices.
Bioidentical Hormone Replacement Therapy Explained
Bioidentical hormone replacement therapy (BHRT) utilizes hormones that are chemically identical to those produced naturally within the human body. Advocates suggest that this structural similarity might lead to improved efficacy and reduced side effects, potentially offering a more “natural” way to treat hormonal imbalances, especially during menopause.
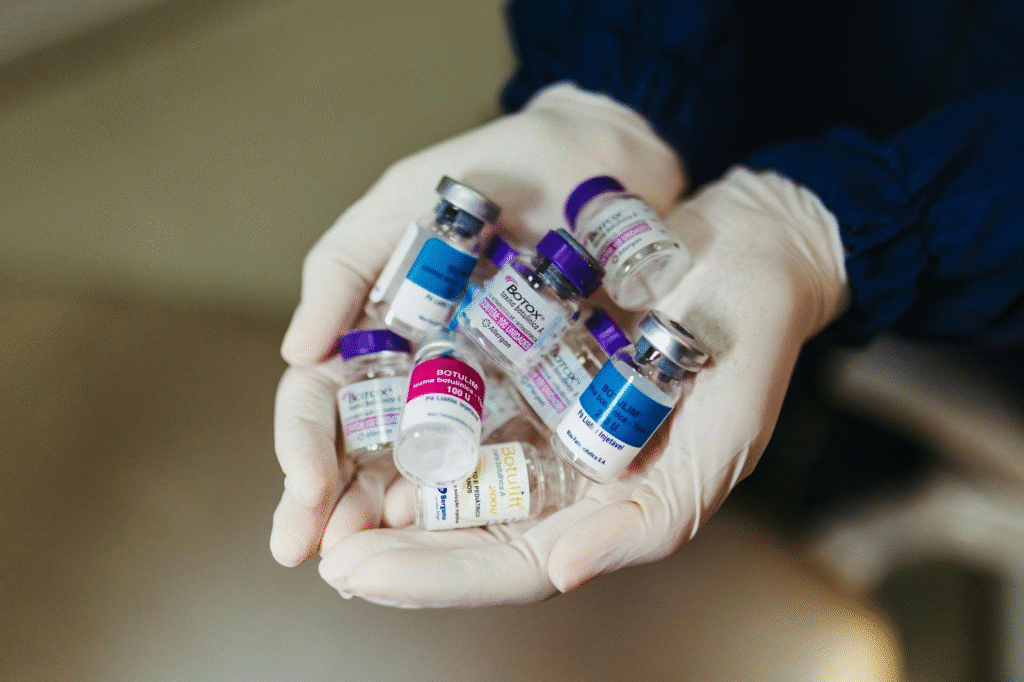
Manufactured from plant estrogens, BHRT hormones are available in various forms, including pills, patches, creams, and injections. bioidentical hormone replacement therapy Facilities such as UCO Medical Clinic in Hallandale Beach often customize dosages to suit each patient’s unique hormonal needs, striving for a tailored treatment approach.
While considering BHRT, it’s advisable to consult with a healthcare professional with expertise in managing hormone health. They can provide actionable guidance on suitable treatment forms, dosages, and monitor hormone levels to ensure optimal benefits.
Traditional Hormone Therapy: An Overview
Traditional hormone therapy, often referred to as hormone replacement therapy (HRT), usually includes synthetic or animal-derived hormones that are not identical to human hormones. These have been used extensively for managing menopausal symptoms and minimizing risks associated with hormone deficiencies, such as osteoporosis.
Conventional HRT can be systemic, affecting the entire body, or localized, such as topical creams and vaginal products focused on alleviating specific symptoms. It has been subject to rigorous scientific scrutiny, particularly concerning its long-term health impacts.
When exploring traditional hormone therapy options, it’s crucial to assess the risks and benefits in concert with medical advice. Experts can assist in determining the appropriate type and regimen, regularly reviewing treatment effectiveness and adjusting therapy as needed.
Comparing Efficacy and Safety: Bioidentical vs. Traditional Hormones
In comparing the efficacy and safety of BHRT and traditional hormone therapy, research suggests no significant difference in symptom relief. However, some patients report improved quality of life and fewer side effects with BHRT, though scientific consensus on this claim is not absolute.
Concerns surrounding the safety of hormone therapies peaked after studies like the Women’s Health Initiative linked traditional HRT to increased risks of certain diseases. Advocates for BHRT argue that its natural composition could lower these risks, though this remains an ongoing area of research.
Whether choosing BHRT or traditional hormone therapy, it’s essential for patients to evaluate the risk-benefit profile and consider personalized advice from healthcare specialists. Regular screening and close medical supervision are key to maintaining safety throughout the course of treatment.
Personalizing Treatment: Factors Influencing Hormone Therapy Choices
The decision between BHRT and traditional hormone therapy often hinges on various personal factors, including a woman’s health history, the severity of symptoms, and lifestyle. Individual hormonal profiles dictate the types and dosages of hormones used in therapy, be it BHRT or traditional.
Genetic predispositions, the presence of chronic conditions, and a patient’s personal treatment preferences should all be discussed with a healthcare provider. Clinics like UCO Medical Clinic offer comprehensive hormone health evaluations to personalize treatment effectively.
Moreover, ongoing research, evolving formulations, and varying regulatory standards continue to shape the landscape of hormone replacement therapies. Staying informed about the latest medical evidence and consulting with a specialized medical team can lead to a more satisfactory treatment experience.
In conclusion, both bioidentical and traditional hormone replacement therapies serve as vital options for women managing the complexities of hormonal changes. A thorough understanding of each approach’s benefits and risks, along with personalized medical guidance, is paramount in choosing the most appropriate and safe treatment. Balancing hormonal health is a dynamic process, and women should feel empowered to seek the options that best align with their wellness goals and bodily harmony.